Posted by Balgowlah_admin in on November 23rd, 2022

Do you have foot, ankle, or lower leg pain? Or perhaps something just doesn’t look or feel right? (e.g. flat feet, bunions, or knock knees). Our Podiatrist, Brendan Coyle, has 20 years’ experience in the field of lower limb biomechanics and is expertly placed to work out what is going on, why it’s happening, and how to fix it.
We’ll perform a biomechanical assessment to identify the source of your pain, provide you with an accurate diagnosis, ascertain the cause and contributing factors, and provide you with a comprehensive treatment plan.
Even in the absence of pain, a biomechanical assessment allows us to identify and address structural and functional lower limb problems to help prevent injury and/or improve performance.
We set aside 1 hour to ensure your pain or problem is assessed and managed without cutting corners. Your appointment will consist of:
The consultation – we set aside the time to listen and understand your concerns and individual requirements. We’ll discuss your presenting concern, injury history, activity levels, goals, expectations, and more. Information collected here helps guide the assessment.
The assessment – we perform a non-weight bearing and weight bearing examination. Your pain or injury will dictate how much we’ll get you moving but, typically, we’ll have you sitting, standing, walking, running, or whatever it takes to identify your problem and any contributing factors. A footwear assessment will also be included in the assessment process.
The diagnosis – you’ll leave with detailed explanations and answers, so that you understand the ins and outs of your pain or injury.In most cases, we’re able to clinically diagnose your pain, however, if it is inconclusive, we can investigate further through scans, tests, or referrals to professionals in our trusted local referral network.
The treatment plan – we will provide you with individualised short-, medium- and long-term solutions. Our goal is to resolve your problem as quickly as possible, but we also need to equip you with long-term strategies to prevent future issues.
Treatment will always include education about your pain or injury and its contributing factors. This is vital for short and long-term management. Other treatment options include:
Posted by Balgowlah_admin in on November 23rd, 2022

When it comes to the world of footwear, one can be easily overwhelmed by choice. Athletic and active footwear has grown leaps and bounds over the past decade. We are experts in this field and can take the guesswork out of picking the right shoe.
Whilst there is no one right shoe for you, we have the experience and knowledge to help significantly narrow down the choice. We can provide advice on:
Footwear has a huge influence on our feet, legs, and bodies in general. The right shoe can have one functioning well and in comfort, whilst the wrong shoe can be a prime contributor to pain, injury, and poor performance.
If you’re attending with pain or injury, a footwear assessment is part of our comprehensive biomechanical assessment. We will assess your footwear both off and on to determine if they are a contributing factor to your problem. You will then be provided with advice and a prescription for new shoes, if required.
In the absence of pain or injury, a close look at your footwear and expert advice on what you should and should not be wearing is important in preventing problems from developing.
Posted by Balgowlah_admin in on November 23rd, 2022

Our Sports Podiatrist, Brendan Coyle, has been prescribing quality custom orthotics for 20 years. He has prescribed orthotics to international rugby players, professional footballers, amateur sportsmen, runners, walkers, and workers alike. He has the experience and knowledge to fit comfortable, functional, and effective foot orthotics, customised to your individual requirements.
Foot orthotics are specially made shoe inserts designed to help heal or prevent injury, relieve pain, address poor biomechanics, and even improve performance.
As we stand, walk, run and move, there are pressures and forces acting on our feet that can contribute to pain or injury. Foot orthotics are used to alter these pressures and forces and can be effective in addressing pains and injuries of the feet, ankles, legs, hips, and back.
Custom orthoses are just that, custom. We can make orthotics that are firm and rigid, soft and flexible, and everything in between. Your orthotics are prescribed, if required, following a thorough biomechanical analysis to determine your individual requirements. We consider your injury history, footwear, foot type, and more, before prescribing your orthotics.
Precision 3D scanning and the most advanced design and manufacture technology is used to ensure your orthotics suit your unique foot shape, biomechanics, footwear, and activity type.
We prescribe:
In many cases, foot orthotics can be avoided. We won’t prescribe custom orthotics if there are effective alternative treatment options, or we believe their benefit to you would be limited. If orthotics are prescribed, seldom are they a stand-alone treatment. Soft tissue programs, footwear advice, activity modification, strappings, paddings, and various other modalities of treatment almost always accompany their prescription.
Whilst orthotics work best in certain shoes, they can be made to fit almost any shoe:
We will give you advice on the footwear best suited to address your pain, injury, and other individual requirements.
At your fitting appointment, we will ensure your orthotics fit well to your feet and your shoes. We will get you standing and walking to ensure they’re comfortable and ready to wear. You will be provided with instructions detailing the first few weeks of their use, and we will discuss any review requirements. Rarely do we have issues with our orthotics, but in the event that there’s something not quite right, we guarantee that these concerns will be addressed and rectified.
Posted by Balgowlah_admin in on November 23rd, 2022

Have an ingrown toenail? Or perhaps your toe is painful and you’re unsure?
At Balgowlah Podiatry, we are experts in the diagnosis and treatment of ingrown toenails, with 20 years’ experience in providing both immediate relief and permanent solutions to this painful condition.
An ingrown toenail, or onychocryptosis, occurs when the corner or side of the nail grows into the adjacent flesh. This can cause redness, swelling, pain and discharge.
There are various reasons why ingrown toenails occur, but commonly they are caused by one or more of the following:
Treatment of your ingrown toenail will depend on its severity. Ingrown toenails rarely improve over time, so the sooner you seek treatment, the better.
We have the skill to quickly and carefully remove the piece of nail that has penetrated the skin with little to no discomfort. However, if the site is painful, then a local anaesthetic can be used.
Once the offending piece of nail is removed, a dressing will be applied, and you will then be given instructions on how to care for your toe at home. Typically, you’ll walk out the door, ready to return to shoes and activity within 1-2 days. You will also be educated on how to best prevent your ingrown toenail from reoccurring.
For those stubborn, recurrent ingrown toenails, we offer simple, safe, and effective, minimally invasive surgical procedures that provide a permanent fix.
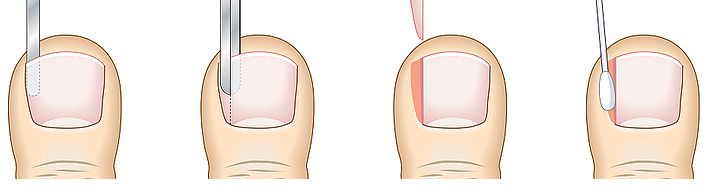
Our surgical procedures are performed in our Balgowlah clinic, under local anaesthetic, and typically take about 1 hour from start to finish. During this procedure, a chemical (Phenol) is applied to the nail root, which prevents any re-growth or recurrence. This is effective in over 95% of cases.
Once complete, you will walk out of the clinic with your toe dressed and instructions on how to care for your toe during the healing process, which is typically 3-4 weeks. During this time, we will ask you to refrain from impact activity (e.g. running and kicking balls) and swimming/getting the toe wet.
This depends on your individual insurance policy. If you have extras containing podiatry cover, it is likely a portion of the fee will be covered.
Posted by Balgowlah_admin in on November 23rd, 2022

Does your child regularly complain of pain in their legs or feet? Are they limping during or after sport?
Children’s legs and feet are not just smaller versions of our own. As they grow and develop, there are key differences which mean children can develop unique pains and injuries.
We know that when your child complains of pain this can be worrying. With 20 years’ experience in paediatric podiatry, we are perfectly placed to diagnose the cause of your child’s pain and provide you with answers. We’ll set aside the time to listen, examine, diagnose, and treat your child in a caring, professional, and friendly environment.
Even in the absence of pain, sometimes things just don’t look right – flat feet, knock knees, bow legs, bunions, and so on. The feet and legs of a growing child are constantly changing. We will educate you and your child on what is normal and what is not, and, if treatment is required, we will provide you with options to suit your child and family’s unique needs.
Active, growing feet should be fitted with the right shoes. We offer advice on casual shoes, school shoes, dance shoes, netball shoes, football boots, and other sports-specific shoes.
If your child is experiencing pain, contact us now for a thorough assessment, detailed answers, and treatment that works.
Posted by Balgowlah_admin in on November 23rd, 2022
We deliver high quality general podiatry services in a professional, caring, and friendly environment
After 20 years working with feet, we’ve seen it all. Some of the common conditions we see and treat on a regular basis include:
Toenail fungus (Onychomycosis) is more common than you may think, affecting about 10% of Australians. Whilst it is not dangerous and rarely causes pain, it is what it does to the appearance of the nail that brings most people to see us. White, yellow, or brown discolouration is common, and, in time, the infected nail will often become thick and brittle.
Toenail fungus can be stubborn and difficult to shake. With 20 years’ experience treating toenail fungus with almost every treatment available (i.e. topical treatments, laser, oral medication, and more) we know what works and what doesn’t. After examining your nails, we will give you honest advice on the best treatment available for your individual case.


Plantar warts (Verruca pedis) are lesions that occur on the bottom of the foot or around the toes and are caused by the Human Papilloma Virus (HPV). They are transmitted from one person to the next through direct contact – either from someone with the virus, or through socks, shoes, or surfaces. A simple wart is not a serious health concern, however they can be very uncomfortable, or even painful, when they present on the weight bearing areas of the feet. Warts can also grow and spread, so early treatment is recommended.
Treatments include medicated pastes and liquids, cryotherapy, and minor surgical procedures for those that are stubborn and persist.
Tinea pedis is a fungal infection of the skin that normally begins between the toes but can occur anywhere on the feet. It is often present in those with sweaty or damp feet, who spend a lot of time in confined footwear. Tinea can present in various forms but typically appears as red, flaky skin that can itch, sting, or burn. In most cases, treatment is straightforward and consists of addressing foot hygiene, footwear advice (shoes, socks, and the materials they are made from), and topical medications.


Calluses and corns are thick, hardened layers of skin caused by friction and pressure. Calluses are spread out over larger areas of skin, generally occur in the weight bearing areas of the feet and may or may not be painful. Corns are similar to calluses but are generally smaller with a hard central core that sits deeper into the healthy skin. Corns are often painful and can occur in the weight bearing areas of the feet as well as in between and on the tops of toes.
The pressure and friction that causes calluses and corns to develop can come from poor fitting footwear, bony prominences, walking and running patterns, and various skin conditions.
Immediate treatment of calluses and corns involves shaving back the thickened skin, and in the case of corns, removing the hard, central core with a scalpel. This treatment is typically quick and painless.
Longer term management involves addressing the causes and contributing factors. This means taking a good look at the structure and function of your feet to address any bony prominences or biomechanical issues. Footwear assessment and advice is also important.
It is recommended that patients with diabetes have their feet assessed every 12 months, or earlier in some cases. This is because people with diabetes have higher risk of developing foot problems due to possible changes in circulation and sensation to the feet.
A diabetes foot health assessment consists of the following:
Following your assessment, we will provide you with advice and treatment to ensure your feet are in the best possible condition and health.
